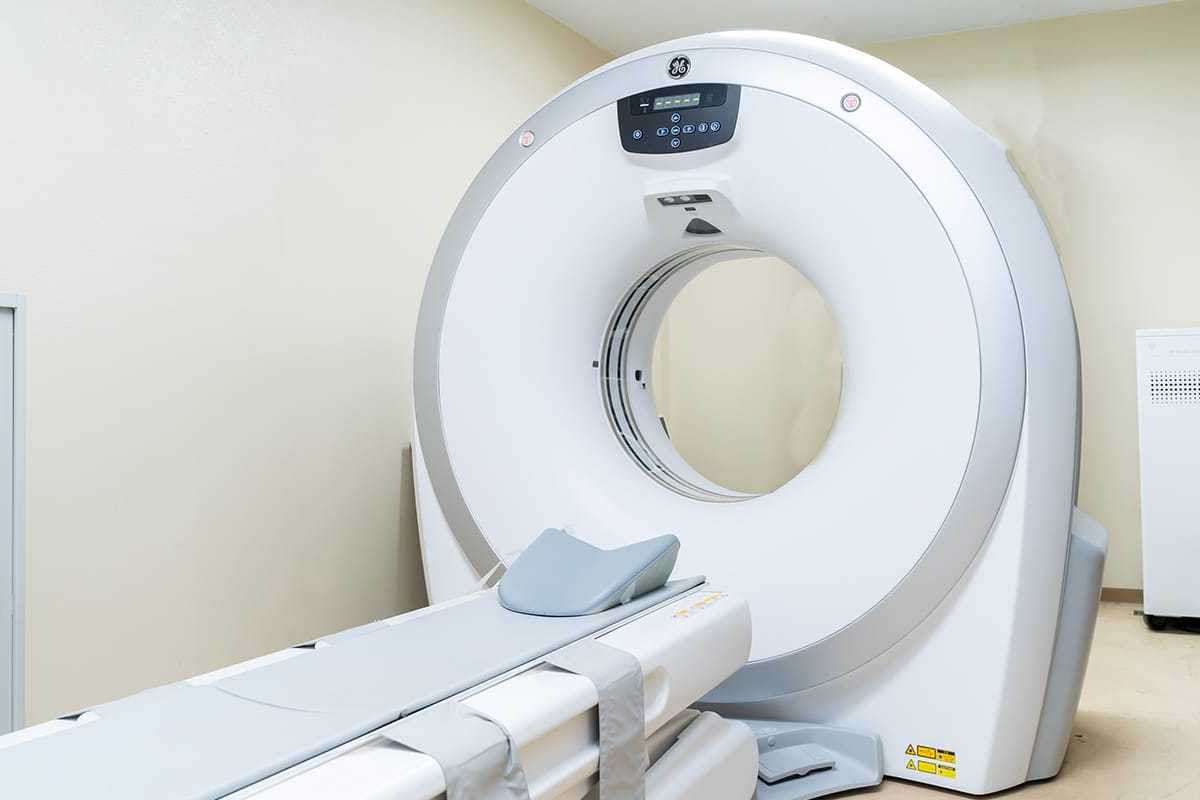
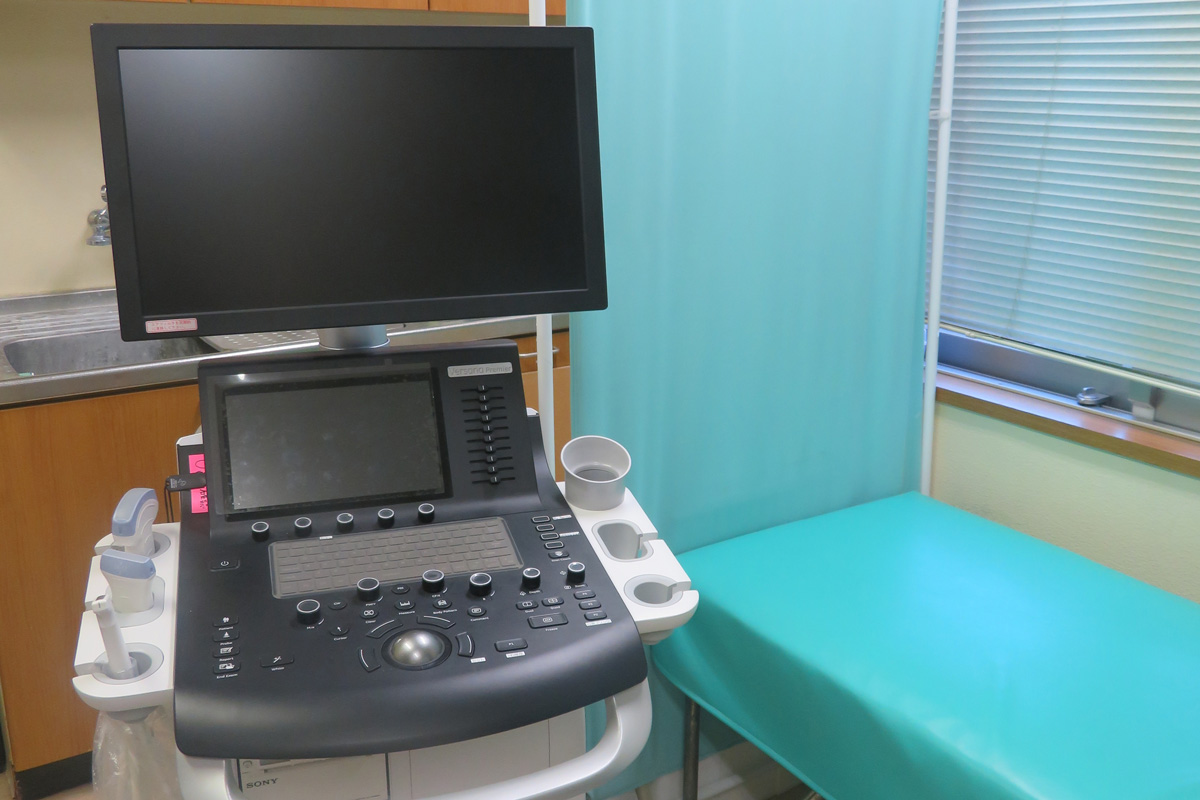
◆エコー検査(頸動脈エコーなど):予約制
エコー検査 ※各日、午前中
【5月】8日(水)・20日(月)
【6月】12日(水)・24日(月)


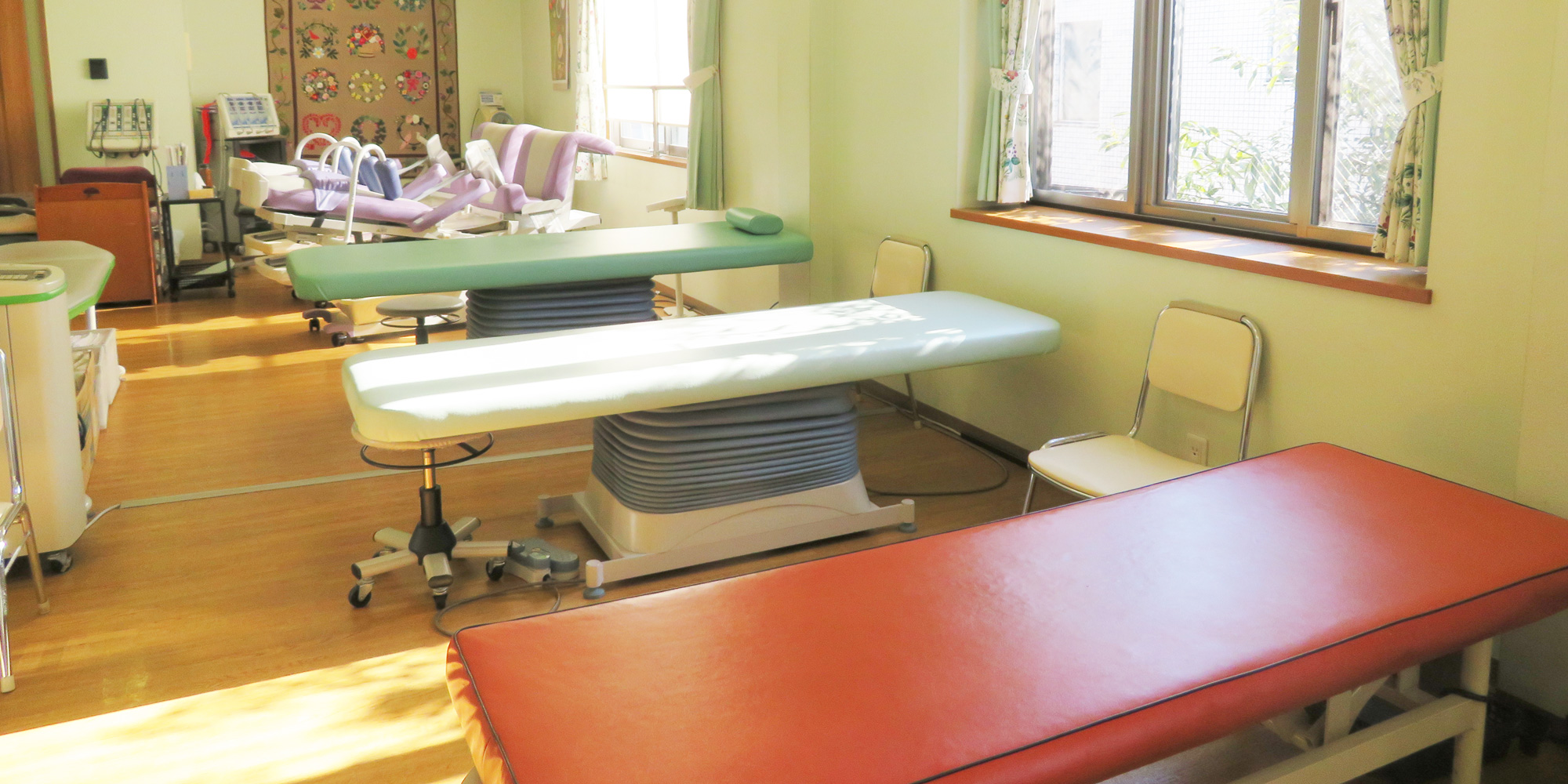
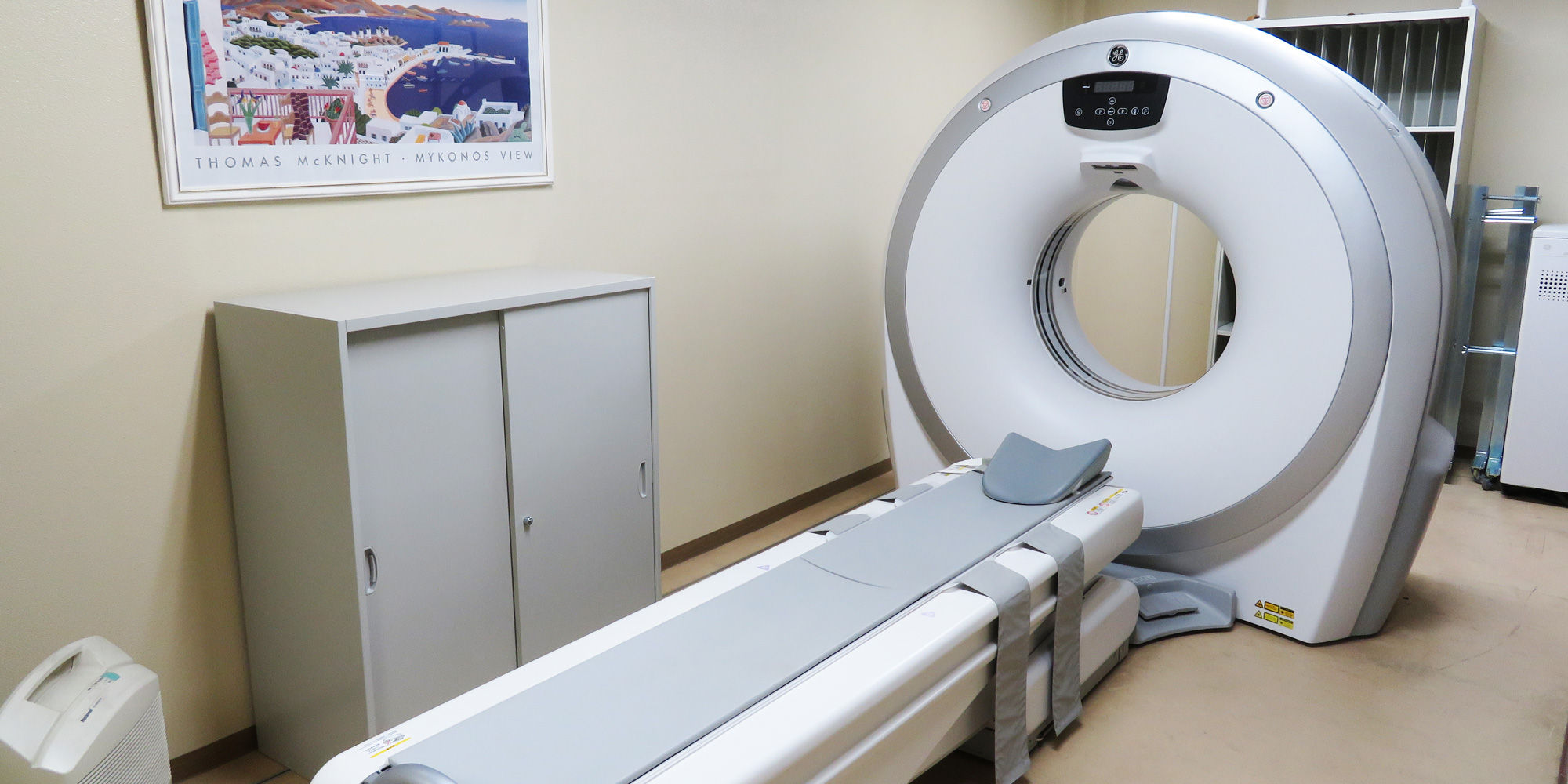
脊椎疾患治療を中心として
皆さまの健康的な生活を支援します。
◆受付時間について◆
受付時間は下記になります。
月~金
午前/8:30~12:00 午後/14:30~17:45
土曜
午前/8:30~12:15
初診の方は午前/12:00、午後/17:30までに
再診の方は午前/12:00、午後/17:45までに
受付をお済ませください。
検査・入院の機会が制約されますので早めのご来院をお願いします。
◆木曜の診察について◆
木曜日の院長の診察は午後からになります。
(午前中は代診医師の診察になります。)
初診の方、新しいご症状でご相談の方は午後からの院長の診察にお越しください。
お知らせ
ごあいさつ
東京都武蔵野市の整形外科、脳神経外科の
安岡整形外科脳外科クリニックです。
当院では、整形外科・脳神経外科・神経内科各科の分化の弊害を取り除き、リハビリテーションを軸とした統合的・包括的な(Comprehensive approach)医療をめざします。また、その基本理念は、個々の患者さまご家族を第一(Best interest of patient)とすることであり、基幹病院との緊密な提携も踏まえてこれを実行して参りましたし、これからもしつづけます。
また、医療環境(Amenity)を重視し、和やかな雰囲気のクリニックをめざします。
クリニック本体の建築にあたっては、災害時医療に対応できるよう耐震性を第一とした工法を採用しております。治療においても介護においても、医学の進歩と社会制度の複雑化による情報洪水の中で、患者さんとご家族が迷路に入ってしまっていることが少なくありません。
当院では職員一体となってご相談を受け、その上で治療と介護をすすめるための指針を提示(Navigator)させていただきます。また寝たきりになってしまう主な要因は脳卒中などの脳血管疾患と転倒による骨折となっており、当院では脳神経外科と整形外科を掲げておりますので、上記の寝たきりの原因に対して治療と予防を行っていくことが可能です。
当院の検査
医院案内

| 月 | 火 | 水 | 木 | 金 | 土 | 日 | 祝 | |
|---|---|---|---|---|---|---|---|---|
| 08:30~12:15 | ● | ● | ● | ● | ● | ▲ | / | / |
| 14:30~18:00 | ● | ● | ● | ● | ● | / | / | / |
▲・・・土曜午前 08:30~12:30
【休診】土曜午後、日曜・祝日
・木曜日の院長の診察は午後からになります(新しい症状等のご相談は午後の
診療時間にお越しください)
・受付は診療終了の15分前までにお願い申し上げます。
・初診(新しい症状)の方は30分以上前に来院して頂きますようご協力お願いします。
交通案内
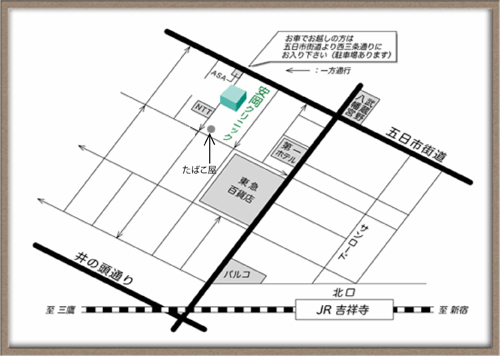
| 最寄駅 | 「吉祥寺駅」北口より徒歩7分 |
|---|---|
| 駐車場 | クリニックビル1F |
| 近くのランドマーク | 吉祥寺東急デパートより徒歩2分、武蔵野NTT斜め向かいにあります。 |